What You Need to Know Before Starting Treatment
Table of Contents:
If you’ve been dealing with chronic back pain, a herniated disc, or sciatica, chances are you’ve come across spinal decompression therapy. It’s often advertised as a non-surgical solution for disc-related pain, but many people still ask the same important question: Does spinal decompression work?
The short answer is: it can — for the right patient and the right condition. But like any treatment, it’s not a magic fix. In this guide, we’ll break down how it works, who it helps, potential risks, and what doctors actually think about it.
What Is Spinal Decompression?
Spinal decompression is a therapy designed to relieve pressure on spinal discs and nerves. It is commonly used for conditions such as:
Herniated or bulging discs
Sciatica
Degenerative disc disease
Chronic lower back pain
Neck pain
Most people referring to this therapy mean non-surgical spinal decompression therapy, not spinal decompression surgery.
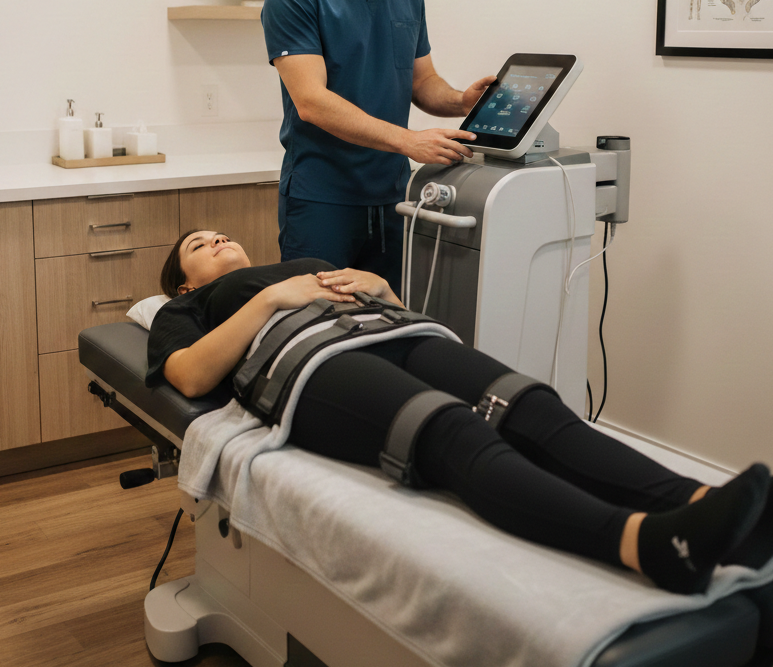
Non-surgical treatment uses a spinal decompression machine or motorized spinal decompression table to gently stretch the spine in controlled cycles. The goal is to create negative pressure within the discs, which may help reduce nerve compression and improve blood flow to injured areas.
How Does Spinal Decompression Therapy Actually Work?
To understand whether spinal decompression works, it helps to understand what’s happening inside the spine.
Between each vertebra sits a disc that acts as a cushion. When discs become compressed, bulge outward, or herniate, they can press on nearby nerves. This pressure often causes:
Lower back pain
Leg pain (sciatica)
Tingling
Numbness
Weakness
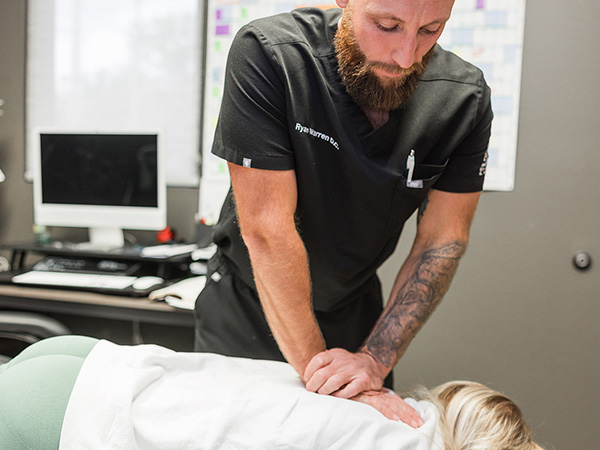
During treatment, you lie comfortably on a spinal decompression table while a harness secures your hips or upper body. The spinal decompression machine then gently stretches and relaxes the spine in cycles.
This stretching is carefully calculated — it’s not the same as simply hanging upside down or doing basic stretches. The therapy aims to:
Reduce disc pressure
Improve circulation
Encourage movement of bulging disc material
Promote natural healing
So when people ask, does spinal decompression work, the answer depends on whether the pain is truly disc-related.
Does Spinal Decompression Work for Herniated Discs?
For patients with confirmed herniated or bulging discs, spinal decompression therapy may provide relief. Decreasing pressure inside the disc, it can reduce irritation on nearby nerves.
Many providers combine decompression with spinal decompression exercises to strengthen supporting muscles. This combination often improves outcomes compared to passive treatment alone.
However, results vary. Some patients experience significant pain reduction, while others notice only mild improvement.
What Is the Success Rate of Spinal Decompression Therapy?
Success rates often depend on:
The severity of the disc injury
How long have symptoms been present
Overall health and lifestyle
Commitment to follow-up exercises
Some clinics report success rates between 70% and 90% for carefully selected patients. That said, independent research shows mixed results. Many studies suggest spinal decompression therapy works best when combined with physical therapy and lifestyle adjustments.
So again, does spinal decompression work? Yes, for many people — but not universally.
Is It Good to Decompress Your Spine?
In the right circumstances, yes.
Decompressing the spine can relieve pressure on nerves and reduce inflammation. For people with chronic disc compression, it may offer a non-surgical alternative before considering more invasive procedures.
However, spinal decompression therapy is not recommended for individuals with:
Severe osteoporosis
Spinal fractures
Advanced spinal instability
Certain surgical implants
A proper evaluation by a licensed provider is essential.
What Are the Negative Effects of Spinal Decompression?
Non-surgical spinal decompression is generally considered safe. Most side effects are mild and temporary, including:
Muscle soreness
Temporary stiffness
Mild increase in pain after early sessions
Serious complications are rare with non-surgical treatment. However, spinal decompression surgery carries greater risks, including infection, bleeding, and a longer recovery time.
If symptoms worsen significantly during therapy, treatment should be reassessed.
Do Doctors Recommend Spinal Decompression?
Opinions vary.
Some chiropractors and spine specialists recommend spinal decompression therapy for patients who want to avoid surgery. If you’re searching for a chiropractor in Fayetteville, AR, or a provider offering spinal decompression, you’ll likely find clinics promoting it as part of a broader treatment plan.
Other physicians may prefer starting with physical therapy, anti-inflammatory medications, or exercise-based care before considering decompression.
Surgery is typically recommended only when conservative options fail or when nerve compression becomes severe.
Spinal Decompression vs. Surgery
It’s important not to confuse non-surgical therapy with spinal decompression surgery.
Non-Surgical Therapy:
Uses a spinal decompression machine
No incisions
Minimal downtime
Performed in outpatient settings
Surgical Decompression:
Removes bone or disc material
Requires anesthesia
Includes recovery time
Reserved for severe cases
For many patients, non-surgical therapy is explored first.
Who Is a Good Candidate?
Spinal decompression therapy may be helpful if you:
Have disc-related back pain
Experience sciatica
Have imaging confirming disc issues
Have not improved with rest or medication
It may not be ideal for pain caused primarily by muscle strain or severe arthritis.
If you’re unsure, consult a qualified provider who performs a full evaluation before recommending treatment.
Does Spinal Decompression Work Long-Term?
Long-term success depends heavily on what happens after treatment.
Spinal decompression therapy can reduce pressure, but lasting improvement requires:
Core strengthening
Posture correction
Regular movement
Weight management
Ongoing spinal decompression exercises
Without supportive habits, pain may return.
Frequently Asked Questions
Is it good to decompress your spine?
For individuals with disc-related nerve compression, decompression can relieve pressure and reduce pain. It’s important to have a professional evaluation first.
What is the success rate of spinal decompression therapy?
Success rates vary, often ranging between 70–90% in selected cases. Results depend on condition severity and overall health.
What are the negative effects of spinal decompression?
Most side effects are mild, such as temporary soreness or stiffness. Serious risks are rare in non-surgical treatment.
Do doctors recommend spinal decompression?
Some do, especially for patients seeking non-surgical options. Others recommend starting with physical therapy first.